Credentialing is a critical step in building and maintaining a successful healthcare practice. It verifies that providers are properly qualified, ensures recognition by insurance networks, and confirms compliance with industry standards. Without a thorough credentialing process, practices risk delayed reimbursements, reduced patient access, and potential regulatory challenges.
Because credentialing involves multiple steps and significant documentation, a credentialing process flow chart is an effective way to streamline the entire system. It provides a clear structure, keeps tasks organized, and helps providers avoid errors that can cause unnecessary delays.
In this article, we will walk through how the medical credentialing process works, why a structured flow chart is valuable, the differences between physician credentialing services and broader medical credentialing services, and the best practices to follow for smooth operations.
Overview of the Medical Credentialing Process
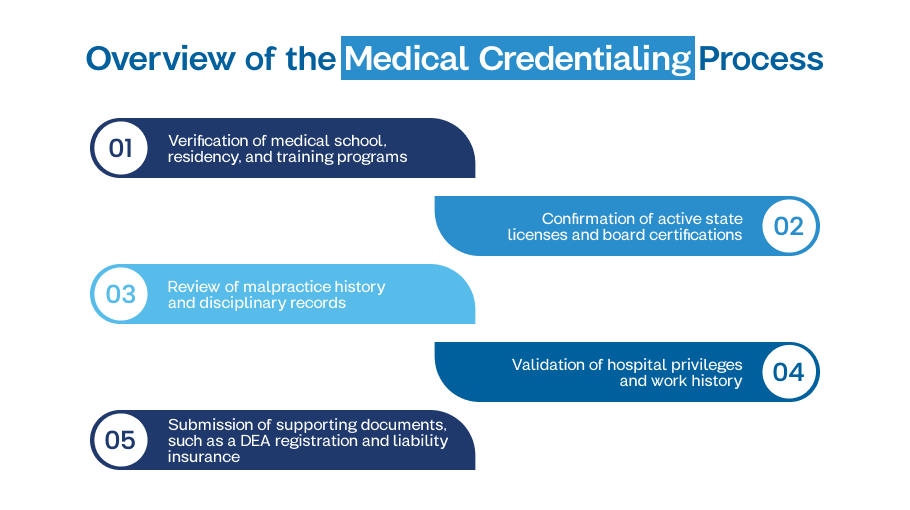
The medical credentialing process is a comprehensive verification system used to confirm a provider’s qualifications, education, and professional history. Insurance networks, hospitals, and regulatory boards require it to ensure that a provider is fully licensed and capable of delivering safe, effective care.
The process typically involves:
- Verification of medical school, residency, and training programs
- Confirmation of active state licenses and board certifications
- Review of malpractice history and disciplinary records
- Validation of hospital privileges and work history
- Submission of supporting documents, such as a DEA registration and liability insurance
Although credentialing is essential, it can be complex and time-consuming. A structured approach makes it easier to manage.
Why Use a Credentialing Process Flow Chart
A credentialing process flow chart breaks down this lengthy process into manageable steps. It provides transparency and consistency, ensuring that no step is overlooked.
Key benefits include:
- Clarity: Everyone involved understands the sequence of tasks.
- Accountability: Responsibilities are clearly defined.
- Efficiency: Tasks are completed in the correct order, reducing delays.
- Compliance: Every provider follows the same standardized process.
For busy practices, this type of structure helps reduce administrative errors and speeds up payer approvals.
Key Steps in the Credentialing Process
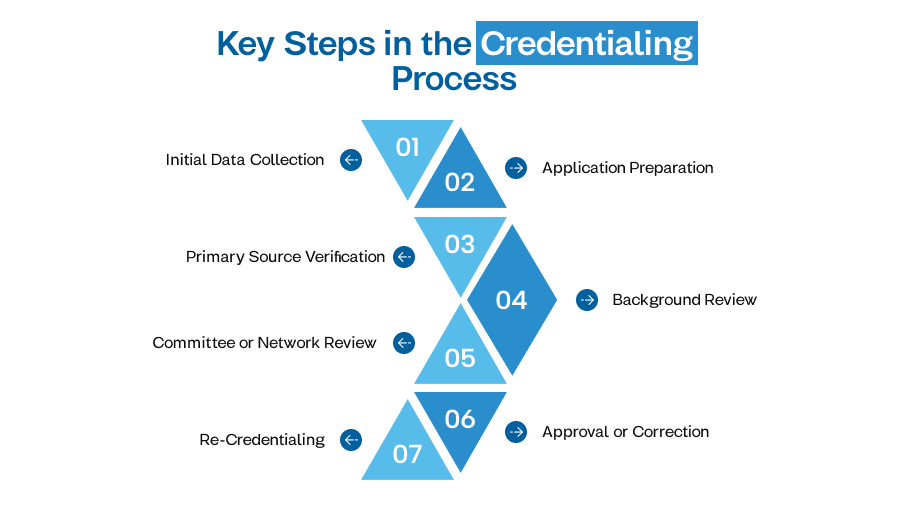
A typical flow chart for credentialing includes the following steps:
-
Initial Data Collection
Gather provider information, including licenses, certifications, malpractice insurance, and professional references.
-
Application Preparation
Complete credentialing applications for insurance companies, hospitals, or networks. Accuracy is critical to avoid delays.
-
Primary Source Verification
Educational institutions, licensing boards, and certification bodies are contacted directly to confirm submitted details.
-
Background Review
Malpractice history, disciplinary actions, and any professional conduct issues are reviewed.
-
Committee or Network Review
Some organizations require a credentialing committee to evaluate applications before approval.
-
Approval or Correction
If everything is verified, providers are approved to join payer networks. If issues are found, additional documentation may be requested.
-
Re-Credentialing
Providers must update their information periodically, often every two to three years, to maintain compliance.
Physician Credentialing Services vs. Medical Credentialing Services
Credentialing support can vary depending on the type of provider.
- Physician Credentialing Services focus exclusively on doctors. They handle requirements for hospital privileges, payer network enrollment, and compliance with physician-specific regulations.
- Medical Credentialing Services cover a broader range of providers, including nurse practitioners, therapists, and allied health professionals. These services are especially valuable for practices with multidisciplinary teams.
Choosing the right service depends on whether a practice needs support for individual physicians or for a wider group of healthcare professionals.
Challenges Practices Face During Credentialing
Despite having a flow chart in place, credentialing is rarely a simple process. Common challenges include:
- Application errors or incompleteness causing delays
- lengthy verification periods, occasionally lasting more than 90 to 120 days
- Regulatory agencies or insurance payers’ shifting requirements
- Provider data entry mistakes, like entering the wrong license number
- Having trouble remembering the re-credentialing deadlines
These challenges can prevent providers from seeing patients and receiving reimbursements on time.
How Credentialing Services Support Providers
Many practices choose to work with specialized medical credentialing services to reduce administrative burden. These services:
- Stay updated on payer and regulatory requirements
- Submit complete, accurate applications to reduce rejections
- Manage communication and follow-ups with payers and institutions
- Scale easily for practices expanding into new networks or states
- Free providers and staff to focus on patient care rather than paperwork
For individual physicians, a dedicated physician credentialing service may be enough. Larger practices benefit from full medical credentialing services that cover multiple provider types.
Best Practices for Enhanced Credentialing
To ensure a smooth credentialing process, healthcare organizations should:
- Begin the credentialing process several months before a provider’s planned start date
- Maintain all provider documents in an organized, centralized system
- Use a flow chart to track applications and monitor progress
- Review every application thoroughly before submission
- Consider outsourcing to professional credentialing services for accuracy and efficiency
- Monitor re-credentialing timelines closely to avoid lapses in compliance
FAQs
-
What is the purpose of medical credentialing?
Medical credentialing verifies a provider’s qualifications, licenses, and background to ensure they meet industry and payer standards for delivering safe patient care.
-
How long does the credentialing process usually take?
Credentialing typically takes 90 to 120 days, but the timeline can vary depending on payer requirements and the accuracy of submitted documents.
-
What’s the difference between physician credentialing services and medical credentialing services?
Physician credentialing services focus only on doctors, while medical credentialing services cover a wider range of providers, including nurse practitioners, therapists, and allied health professionals.
-
How often do providers need to be re-credentialed?
Most providers must update their credentials every two to three years to maintain compliance with payers and regulatory agencies.
-
Why should practices consider outsourcing credentialing?
Outsourcing reduces administrative errors, speeds up approvals, ensures compliance, and frees providers and staff to focus more on patient care instead of paperwork.
Final Thoughts
Credentialing is a cornerstone of healthcare operations. A well-designed credentialing process flow chart ensures every step is completed accurately and on time, reducing errors and unnecessary delays. Pairing this structure with support from experienced medical credentialing services or dedicated physician credentialing services allows providers to keep revenue flowing while maintaining compliance. When the process runs smoothly, providers gain the freedom to prioritize patient outcomes and build stronger relationships.