It is a common understanding among many medical providers that managing healthcare finances manually is a simple task. Let’s give you the hard truth: It’s not! This is because the healthcare process, particularly in the U.S., is not straightforward.
Insurance companies use slow, messy claim submission processes and often deny or underpay claims. With reimbursements shrinking each year, every payment becomes more important! Recent industry reporting has shown increased denial activity and pressure on receivables, which highlights the need for disciplined, measurable revenue cycle management in healthcare.
This post will discuss the basics of revenue cycle management in medical practices, including its key steps, the importance of engaging with reliable revenue cycle management services, and some practical tips and practices for healthcare providers.
Defining Revenue Cycle Management in Healthcare
Well-managed financial operations are vital to safe, continuous patient care. Revenue cycle management in medical practices refers to the administrative and financial tasks that capture healthcare service delivery, file claims, secure payments, and settle accounts.
For clinics and physician practices, the revenue cycle determines how quickly services convert to revenue, how much administrative labor is required, and how adaptable the practice is to payer complexity.
Stages of Healthcare Revenue Cycle Management
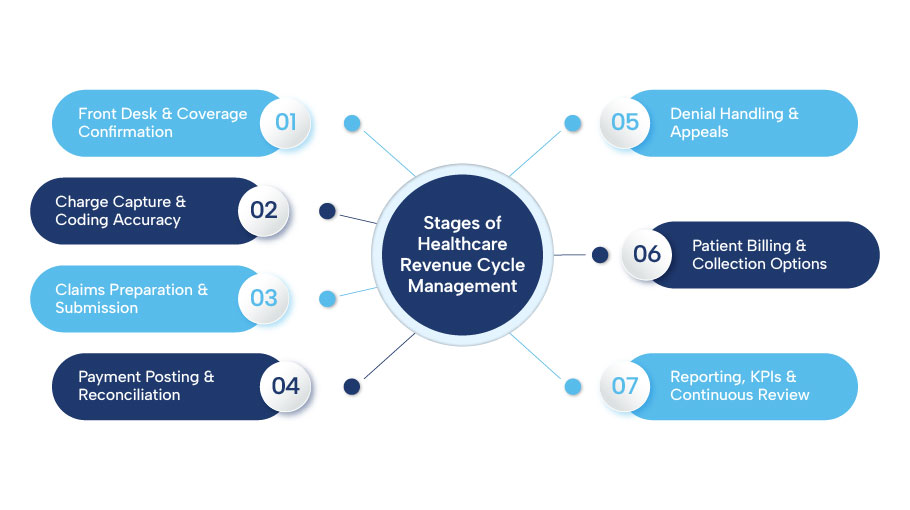
Understanding the important steps of revenue cycle management helps focus on the following improvements:
-
Front Desk & Coverage Confirmation
Collect complete patient demographics, eligibility, and authorization requirements before care or scheduling high-cost procedures.
-
Charge Capture & Coding Accuracy
Convert diagnostics and treatments into CPT and ICD codes. Accurate charge capture prevents lost revenue and reduces downstream corrections.
-
Claims Preparation & Submission
Claims are built, scrubbed for errors, and electronically submitted. Clean-claim rates and batch validation minimize rejections.
-
Payment Posting & reconciliation
Electronic remittance advice (ERA) is posted to patient ledgers. Reconciliation prevents misapplied payments and ageing errors.
-
Denial Handling & Appeals
Responding rapidly to denials by recoverable value, assembling documentation, and filing appeals recovers revenue and limits accounts receivable aging.
-
Patient Billing & Collection Options
Transparent bills, flexible payment plans, and digital payment options improve patient satisfaction and reduce outstanding balances.
-
Reporting, KPIs & Continuous Review
Track metrics such as days in accounts receivable, denial rate, net collection rate, and clean-claim percentage. These data points guide resource allocation and policy decisions.
What Revenue Cycle Management Services Deliver for Practices
When practices engage third-party healthcare revenue cycle management services, vendors typically offer a bundle of capabilities:
- Pre-visit eligibility checks and prior-authorization support
- Certified coding and charge capture specialists
- Claims scrubbing, submission, and payer follow-up
- Denial resolution teams and appeals management
- Patient-payment platforms and statement management
- KPI dashboards, aging reports, and recovery analytics
Many practices adopt hybrid approaches, such as in-house intake and patient relations, with external teams handling complex denials or coding reviews. Industry surveys in 2024–2025 show growing adoption of these hybrid models as practices seek both control and specialist support.
Measurable Benefits of Professional RCM Services Medical Practices Can Expect
Engaging healthcare revenue cycle management services can help deliver measurable outcomes:
-
Faster Cash Collection
Quicker claim submission and consistent follow-up shorten the time between service and payment, improving operating cash flow. This reduces delays in accounts receivable, so practices have cash available sooner for payroll, supplies, and reinvestment.
-
Fewer Denials
Automated claim scrubbing and pre-visit authorization checks catch errors before submission, lowering the chance of rejection. Fewer denials mean less rework and higher clean-claim rates, which directly increase collected revenue.
-
Lower Administrative Load
Automated RCM tasks free billing staff from repetitive rework and manual chasing of claims. Staff can redirect time toward patient-facing duties or higher-value tasks, improving productivity and morale.
-
Improved Patient Payment Rates
Patient portals, online pay links, and structured payment plans make it easier for patients to settle balances at or after a visit. Higher convenience and clear billing lead to increased point-of-service payments and fewer outstanding patient balances.
-
Better Forecasting
Regular KPI reporting and accounts receivable analytics provide predictable trends on cash flow, denials, and payer behavior. With timely data, healthcare leaders can set realistic revenue targets, allocate resources, and make informed budget decisions.
Practical Steps for Strengthening the Revenue Management Cycle in Healthcare
Small steps that can create an immediate impact on the revenue management cycle are as follows:
- Require eligibility checks before scheduling elective procedures. Flag coverage gaps early.
- Run a focused coding audit on your top 20 billing codes to find systematic errors.
- Prioritize denials by dollar value and appeal high-value cases first.
- Enable an online bill-pay portal and automated reminders to reduce patient-side friction.
- Set weekly KPI reviews for denials, days in accounts receivable, and clean-claim rates.
- These operational actions reduce revenue loss and enable management decisions based on obtained data.
What You Should Ask Before Signing Up with an RCM Service Provider
When you vet revenue cycle management services, request clear answers and performance metrics. Here’s a checklist that you can use:
- Can you provide specialty-specific references and measurable case studies?
- What are the expected clean-claim and denial-resolution targets?
- What turnaround times do you guarantee for denial triage and appeals?
- How is data protected, and will you sign a Business Associate Agreement?
- What are all the fees (implementation, monthly, transaction, or success-based)?
Well-structured contracts include KPI-based service levels, escalation procedures, and regular reporting procedures.
The Next Steps
Healthcare Revenue cycle is the financial backbone of clinical operations. Choosing appropriate technology, refining workflows, and, where helpful, engaging with trusted RCM services allows practices to reduce denials, shorten receivable days, and stabilize cash flow.
For practices that need specialized lien recovery or collections expertise, PureMD provides targeted medical collections and lien services that complement internal billing operations. Get in touch with us to learn how we support provider revenue and recovery to deliver an efficient revenue cycle management process.
FAQs
1. What is an effective frequency for KPI review meetings?
A weekly operational huddle reviewing denial trends and accounts receivable aging, paired with a monthly leadership review for cash-flow forecasting, balances immediate fixes with strategic planning.
2. How do lien and workers’ compensation claims change RCM priorities?
Lien and workers’ compensation matters often require longer lifecycle management, legal coordination, and specialized documentation. These cases benefit from vendors skilled in legal follow-up and lien recovery workflows.
3. Which staffing roles yield the greatest ROI when added to in-house teams?
A dedicated denial analyst and a patient-financial counselor typically offer high returns. Analysts recover payer revenue while counselors improve point-of-service collections and reduce bad debt.
4. What compliance evidence should practices require from RCM providers?
Request a signed Business Associate Agreement, SOC 2 attestation or equivalent security summary, encryption standards for data at rest and in transit, and descriptions of disaster-recovery plans.
5. What’s the role of a patient financial counselor, and how can they help my practice?
A patient financial counselor talks with patients before or after visits to explain costs, verify benefits, and set up payment plans so bills are clear and manageable. Having one staff member focused on financial conversations increases point-of-service collections, lowers unpaid balances, and reduces billing calls.